“The initial, rapid response to infections and tissue damage is called acute inflammation”.
- It typically develops within minutes or hours and is of short duration, lasting for several hours or a few days.
- Its main characteristics are the exudation of fluid and plasma proteins (edema) and the emigration of leukocytes, predominantly neutrophils (also called polymorphonuclear leukocytes).
- When acute inflammation achieves its desired goal of eliminating the offenders, the reaction subsides and residual injury is repaired.
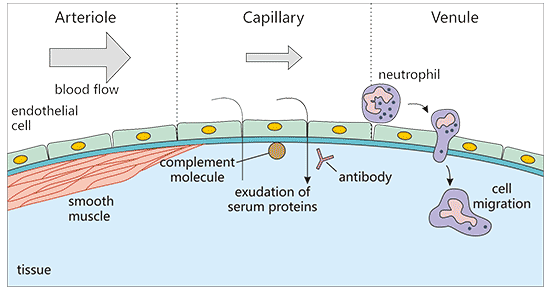
Components of Acute Inflammation:
Acute inflammation has three major components:
- Dilation of small vessels, leading to an increase in blood flow.
- Increased permeability of the microvasculature, enabling plasma proteins and leukocytes to leave the circulation.
- Emigration of the leukocytes from the microcirculation, their accumulation in the focus of injury, and their activation to eliminate the offending agent.
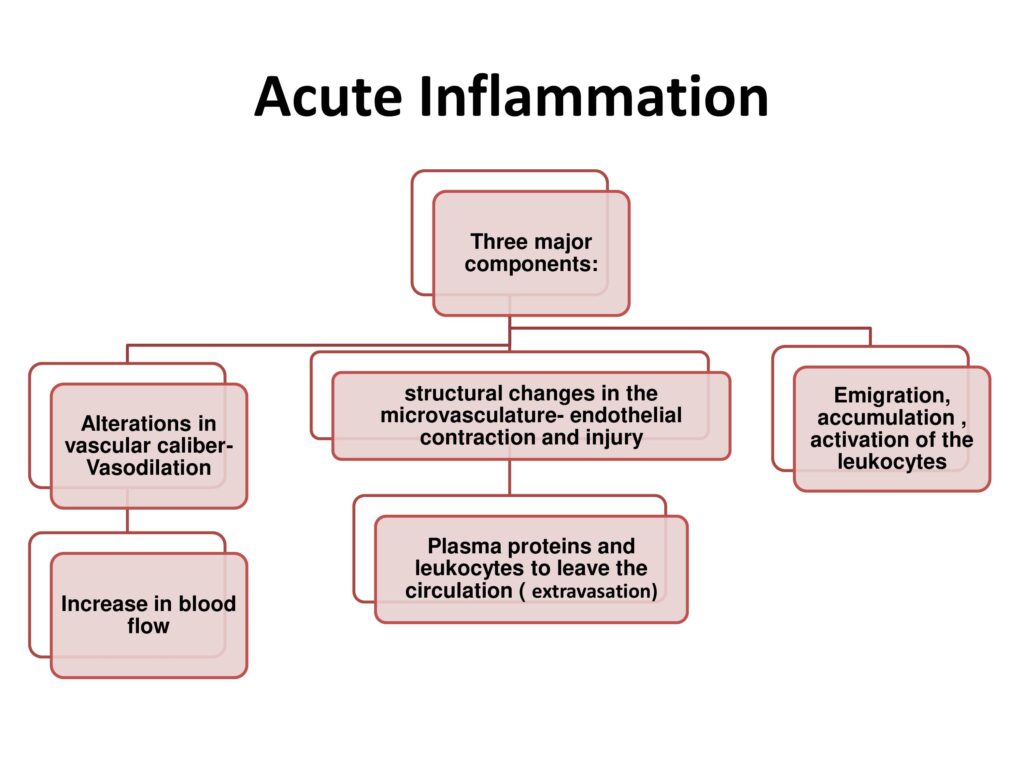
- Vascular changes:
-Increased blood flow (vasodilation)
-Increased vascular permeability
-In addition; endothelial cells are activated, resulting in increased adhesion of leukocytes and migration of the leukocytes through the vessel wall.
- Cellular events:
-Cellular recruitment
-Principle leukocytes in acute inflammation are neutrophils.
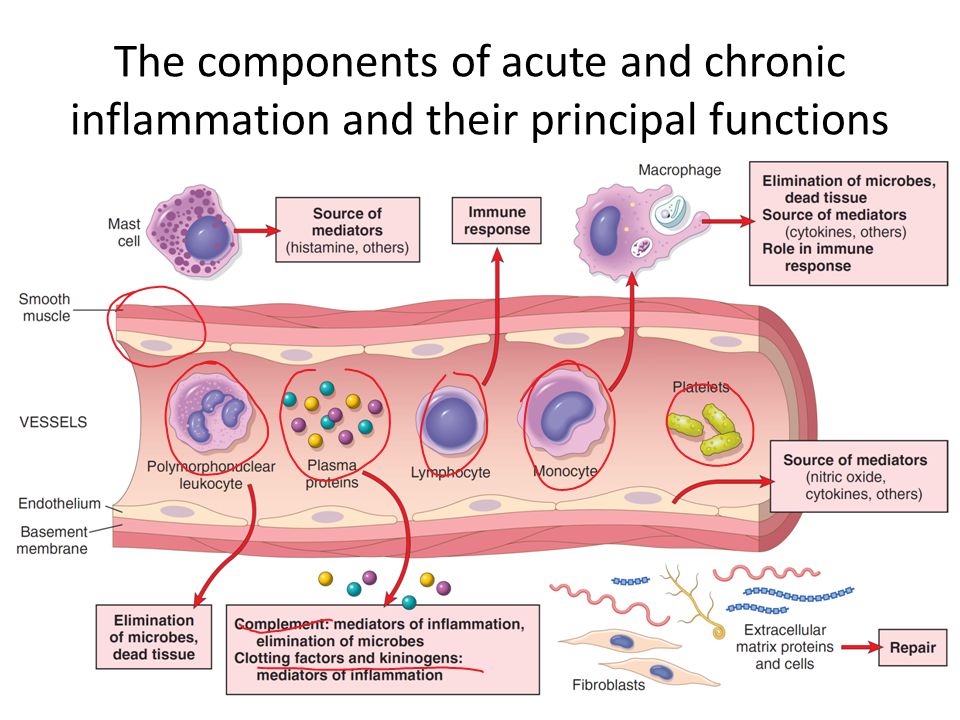
Vascular Changes in Acute Inflammation:
The main vascular reactions are;
- Increased blood flow sec to vasodilation.
- Increased vascular permeability.
Both of these bring blood cells and proteins to sites of infection or injury.
Changes in vascular caliber and flow:
Initial transient vasoconstriction:
- Earliest response to acute injury.
- Lasts only for seconds.
- Transient constriction in the small blood vessels (terminal arterioles).
Persistent vasodilation:
- Occurs rapidly after initial constriction.
- Persists for longer duration.
- Vascular expansion is the cause of redness (erythema) and warmth; the characteristics of acute inflammation, and as two of cardinal signs of inflammation.
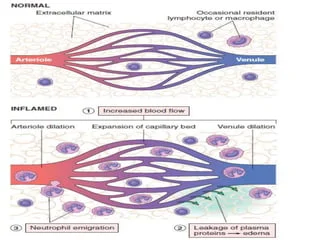
Microvasculature’s:
- Microvasculature becomes more permeable and protein-rich fluid moves into the extravascular tissues.
- This causes red cells in the flowing blood to become more concentrated, thereby increasing the viscosity of blood and slowing the circulation.
- These changes can be seen microscopically as “numerous dilated small vessels packed with red blood cells” called Stasis.
Stasis:
- As stasis develops, margination occurs.
“Leukocytes (principally neutrophils) begin to accumulate along the vascular endothelial surface”.
Increased vascular permeability:
- Increasing vascular permeability leads to ‘movement of protein-rich fluid and even blood cells into the extravascular tissues’.
- This results in increased interstitial fluid, leading to more outflow of water of blood in the tissues.
- In acute inflammation, there is marked increase in permeability of capillaries and venules due to active contraction of actin filaments in endothelial cells.
- As a result widening of intercellular junctions occurs, which allows the passage of large amount of fluid and high molecular weight proteins, this process is called exudation and the fluid is called exudate.
- This exudation of fluid produces tissue swelling called inflammatory edema.
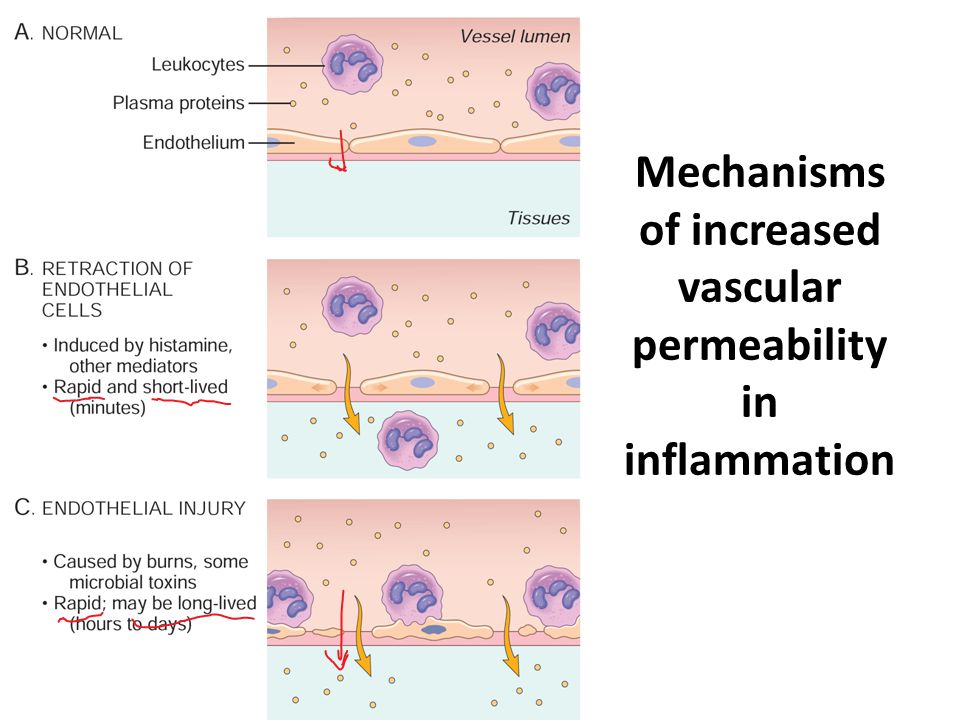
Mechanism of increased vascular permeability:
Possible mechanism of increased vascular permeability;
1.Endothelial contraction:
- Due to actin filament contraction in endothelial cells.
- Leads to intercellular gaps.
- Endothelial injury:
- Due to burns and some infections.
- Results in endothelial cell necrosis.
- Leads to vascular leakage.
- Leukocyte mediated endothelial injury:
- Due to release of proteolytic enzymes from leukocytes, which accumulate during inflammatory response.
- Leakage from new blood vessels:
- These new blood vessels remain leaky until the proliferating endothelial cells mature sufficiently to form intercellular junctions.
Response of lymphatic vessels:
- In inflammation, lymph flow is increased and helps drain edema fluid, leukocytes, and cell debris from extravascular space.
- In severe inflammatory reactions (esp to microbes), the lymphatics may transport the offending agent, contributing to its dissemination.
Lymphangitis:
- Inflammation of lymphatic system.
Lymphadenitis:
- Inflammation of one or more lymph nodes.
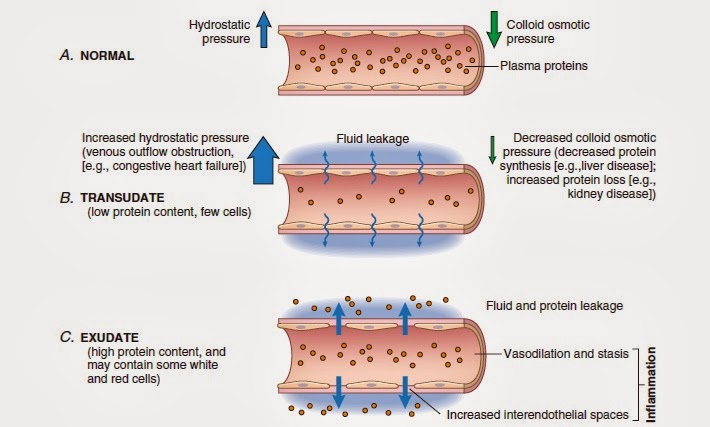
Difference b/w transudate and exudate:
Features | Transudate | Exudate |
Def | “Fluid leaks out of vessels b/c of increased hydrostatic pressure and decreased osmotic pressure”. Ultrafiltrate of plasma | “Fluid leaks out of vessels b/c of increased vascular permeability and increased interendothelial spaces”. Inflammatory extravascular fluid |
Color | Clear | Turbid |
Protein content | Low | High |
Specific gravity | Less than 1.012 | Greater than 1.012 |
Nature | Non-inflammatory | Inflammatory |
Cells | Few | Some; WBC, and RBCs |
Coagubility | Absent (due to lack of fibrinogen) | Present (due to presence of fibrinogen) |
Cellular Events in Acute Inflammation:
Cellular event involves;
1.Leukocyte recruitment
2.Leukocyte activation
- A critical function of inflammation is the delivery of leukocytes (inflammatory cells) to the site of injury to combat infection.
- Neutrophils are prominent cells in acute inflammation, while the lymphocytes, macrophages and plasma cells are prominent in chronic inflammation.
1. Leukocyte recruitment:
Leukocyte recruitment from vascular lumen to extravascular space consists of following sequential events;
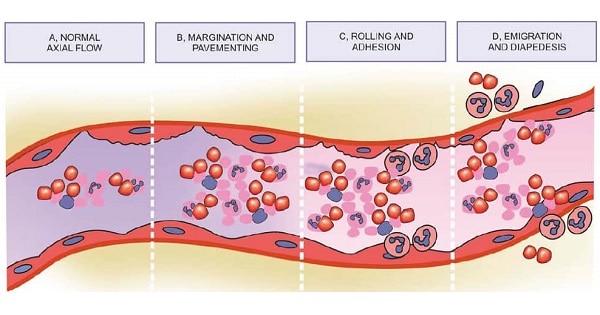
1.Margination and rolling; along the vessels
2.Adhesion; to the endothelium
3.Transmigration; b/w endothelial cells
4.Migration in interstitial tissues; towards chemotactic stimulus
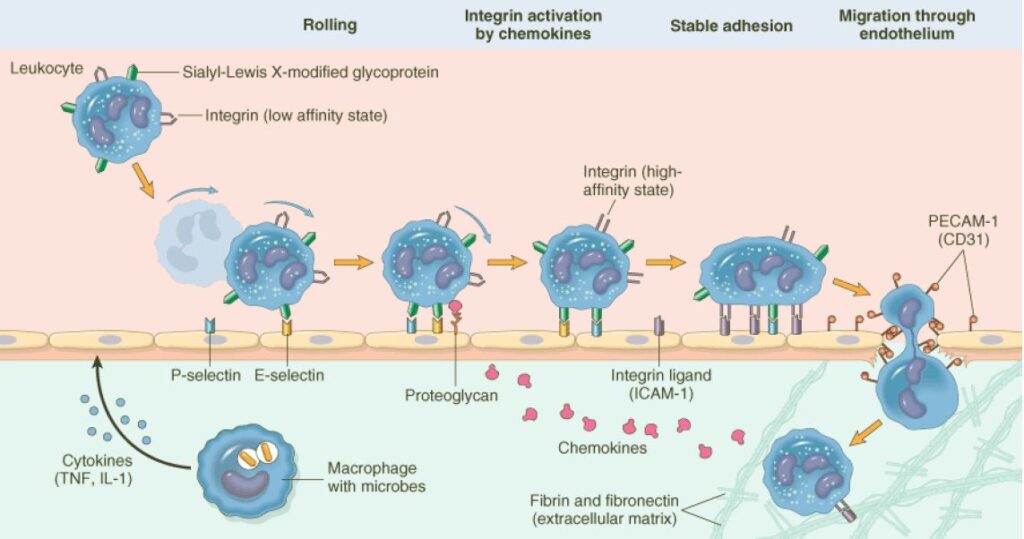
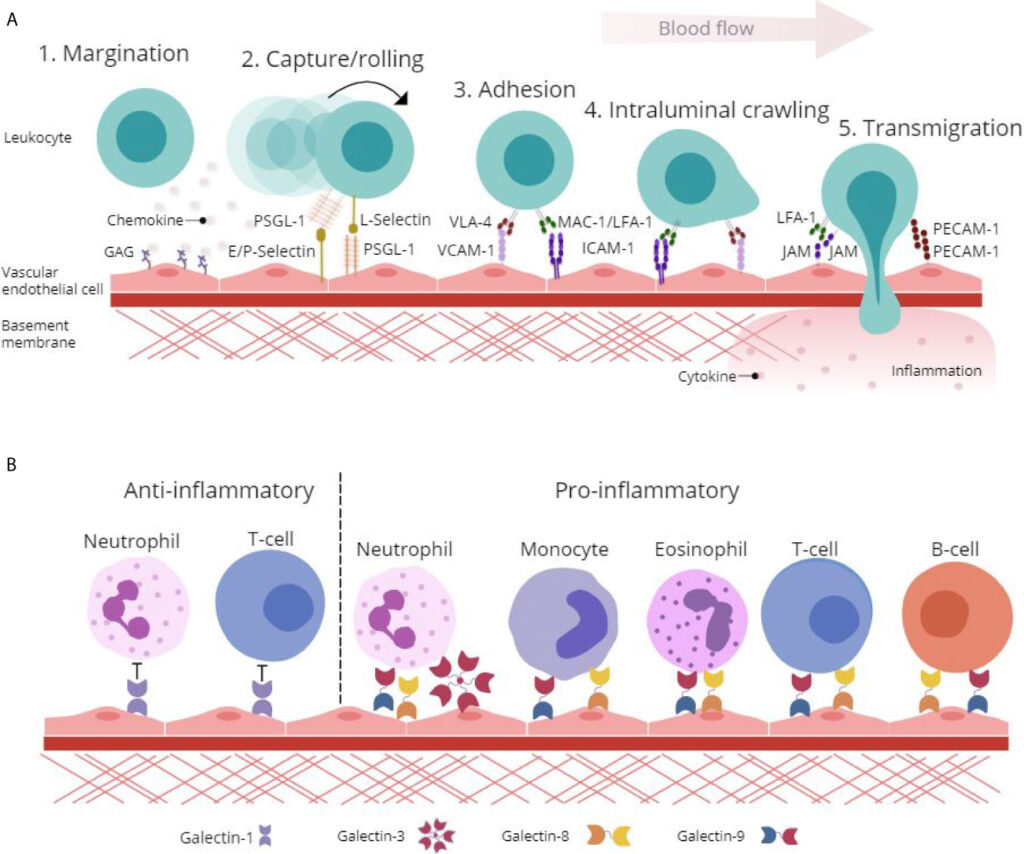
Margination and Rolling:
“Accumulation of leukocytes at the periphery of vessels, called margination”
“The process in which leukocytes binds and detach and thus begin to tumble on endothelial surface, called rolling”
- Binding of leukocytes is largely restricted to endothelium at sites of infection or tissue injury
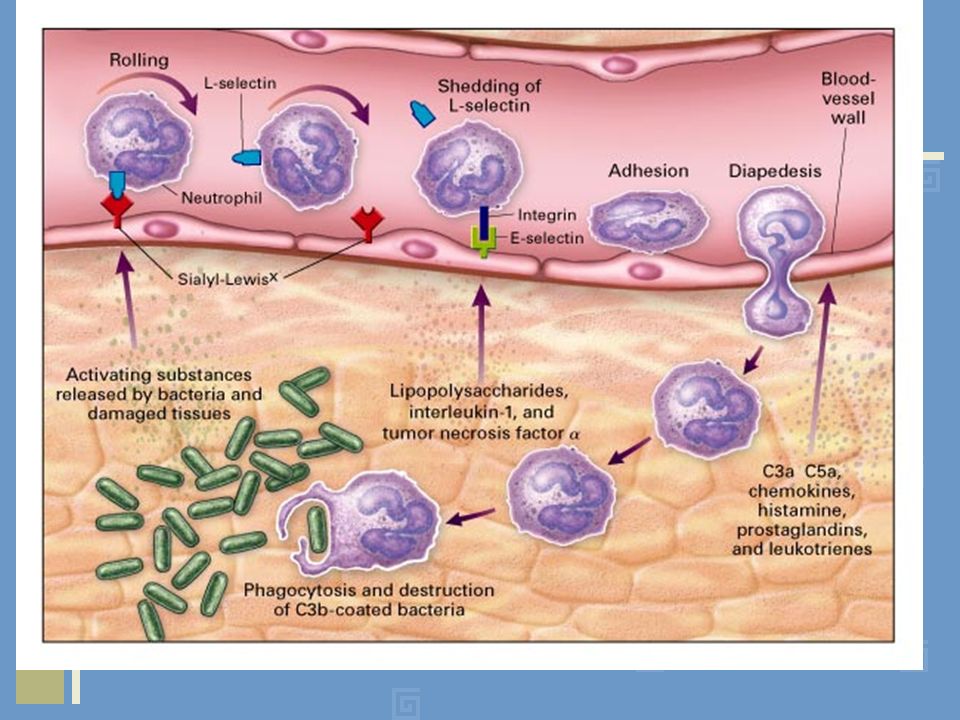
Selectin:
“Receptors expressed on leukocytes and endothelium”
- Family of adhesion molecules.
- Three members of this family are;
-E-selectin; expressed on endothelial cells.
-P-selectin; expressed on platelets and endothelium.
-L-selectin; expressed on most leukocytes.
Adhesion:
“The process which involves firm adhesion of leukocytes to endothelial surfaces, called adhesion”.
- Mediated by integrins (expressed on leukocytes cell surface) interacting with their ligands on endothelial cells.
- Engagement of integrins by their ligands deliver signals to leukocytes that leads to cytoskeletal changes that mediate firm attachment to substrate.
Transmigration:
“Process in which leukocyte interact with PECAM (Platelet Endothelial Cell Adhesion Molecule) proteins, found on the leukocyte and endothelial cell surfaces, which effectively pull the cell through the endothelium, called transmigration”.
Diapedesis:
- “Extravasation of leukocytes, called diapedesis”.
- PECAM expressed on leukocytes and endothelial cells, mediates their binding events needed for leukocytes to traverse the endothelium.

Chemotaxis:
“Movement of leukocytes towards the site of infection or injury along a chemical gradient, called chemotaxis”.
Some chemotactic substances are;
-Bacterial products
-Cytokines
-Components of complement system, particularly C5
-Arachidonic acid metabolites, particularly leukotriene B4 (LTB4)
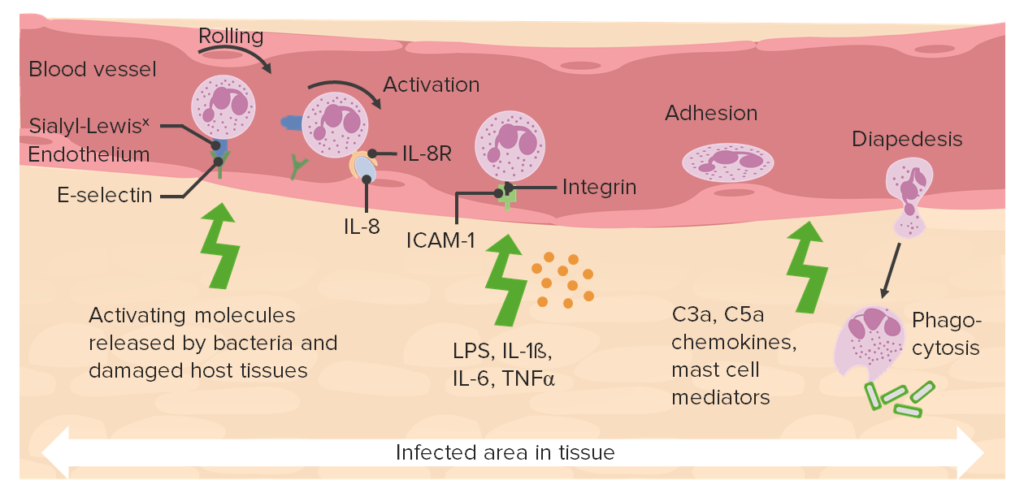
- In most of acute inflammation, neutrophils predominant in the inflammatory infiltrate during the first 6 to 24 hours and are replaced by monocytes in 24 to 48 hours.
- Why neutrophils are predominant???
-Most numerous leukocytes
-Respond more rapidly to chemokines
-May attach more firmly to the adhesion molecules
-After entering the tissues, neutrophils are short lived, they die by apoptosis and disappear within 24 to 48 hours
- In infections (caused by Pseudomonas organisms); cellular infiltrate is dominated by continuously recruited neutrophils for several days.
- In infections (caused by viral infections); lymphocytes may be the first cells to arrive.
- In some hypersensitivity reactions, eosinophils may be the first main cell types.
2. Leukocyte activation:
- Once leukocyte have been recruited to site of infection or tissue necrosis, they must be activated to perform their functions.
- Stimuli for activation; microbes, products of necrotic cells and several mediators.
Leukocyte activation results in the enhancement of following functions;
- Phagocytes of particles.
- Intracellular destruction of phagocytosed microbes and dead cells, by substances produced in phagosomes including ROS, nitrogen species and lysosomal enzymes.
- Liberation of substances that destroy extracellular microbes and dead tissues.
-Neutrophils destroy extracellular microbes.
- Production of mediators including arachidonic acid metabolites and cytokines, that amplify the inflammatory reaction by recruiting and activating more leukocytes.
Phagocytosis:
Process by which the microorganisms and other foreign particles are engulfed and destroyed by neutrophils and macrophages”.
Steps:
- Recognition and attachment of the particles to the ingesting leukocytes.
- Engulfment with subsequent formation of phagocytic vacuole.
- Killing and degradation of the ingested particles.
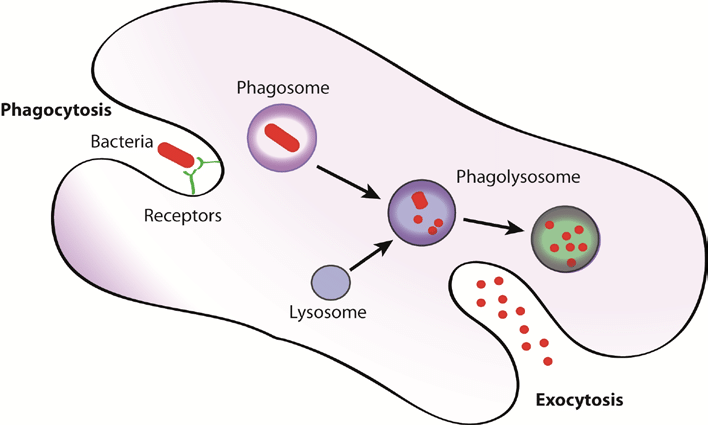
- Recognition and attachment:
- In this process, the white cells identify the object which they have to phagocytize.
- Recognition and attachment of most of the microorganisms is facilitated by coating them with serum proteins called opsonins, which in turn bind to the specific receptors on the leukocytes.
- The opsonins are C3b and IgG.
- Engulfment:
- This process occurs by pseudopodial extensions of the leukocyte cytoplasm which completely enclose the foreign particles, forming phagosome.
- Membrane of lysosomal granules fuse with it and form phagolysosome.
- Lysosomes discharge their contents into phagolysosome causing killing and degradation of microorganism.
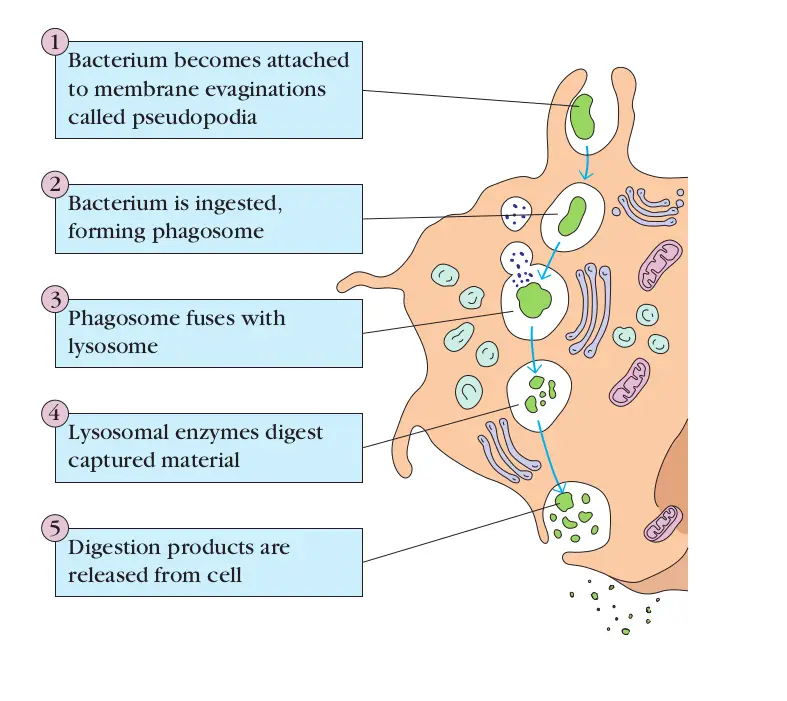
- Killing and degradation:
Oxygen dependent mechanism
- Contact between neutrophil and particulate stimulus leads to activation of a membrane enzyme called NADPH oxidase.
- This enzyme oxidizes NADPH to NADP+H and this process reduces O2 to superoxide anion.
- In the phagosome, superoxide anion ais converted to H2O2.
- H2O2 reacts chloride in the presence of enzyme myeloperoxidase to form hypochlorous radical, which is powerful antimicrobial agent.
- The dead microorganisms are then degraded by lysosomal acid hydrolase enzymes.
Oxygen independent mechanism:
- In the absence of an oxygen dependent system, leukocyte can kill bacterial and other infectious agents by the bactericidal agents (enzymes) produced by the leukocyte granules such as:
-Defensins
-Lysosomes
-Proteases
-Lactoferrin
-Hydrolases

Leave a Reply